The Hidden $300K Problem in Long-Term Care Compliance
FLTCA era has created a perfect storm: tighter enforcement, higher penalties, and inspection expectations that most homes are still trying to manage with tools built for 2010, not 2026.
The author has extensive experience in building predictive analytics for long term care homes
9/7/20247 min read
When the Fixing Long-Term Care Act, 2021 (FLTCA) came into force, it promised stronger accountability, better resident protections, and more consistent enforcement across Ontario. It also quietly introduced a new level of administrative complexity that many LTC homes underestimated—until the first serious inspection cycle under the new regime.
In practice, the cost isn't just fines or public reports. It's the invisible drag on your organization: the hours your best leaders spend parsing inspection reports, coordinating responses, and manually proving compliance instead of improving care.
After working with LTC administrators, DOCs, and executive teams across Ontario, I've watched inspection response evolve from a manageable quarterly task into an always-on, high-stakes, operational discipline. The sector is being asked to operate with the precision of a regulated utility—while still running on spreadsheets, shared drives, and heroic effort.
Where the $120K–$310K Really Goes
Most teams feel the pain of compliance, but very few have actually put a number to it. Here's how the hidden cost adds up for a typical home.
⚠️ Direct labour time
• 20–40 hours per inspection report just to extract, categorize, and interpret findings.
• 300+ hours per year preparing for audits, building action plans, and coordinating responses.
• 520+ hours tracking remediation and follow-up across nursing, IPAC, dietary, environmental, and leadership.
That's roughly 972 hours a year—easily $40,000–$60,000 when you factor in leadership and clinical salaries.
⚠️ Risk and penalty exposure
• Under FLTCA, inspectors and the Director can escalate from written notifications to compliance orders, administrative monetary penalties (AMPs), and, in serious or repeat cases, license actions.
• Administrative penalties and offence fines now reach into the tens or even hundreds of thousands of dollars per non-compliance.
• Maximum offence fines have been doubled compared to the previous framework, with up to $200,000 for individuals on a first offence, $400,000 for subsequent offences, and up to $500,000 then $1,000,000 for corporations in some cases.
For many homes, realistic annual exposure sits somewhere between $50,000 and $200,000 when you consider the cumulative impact of repeat findings, orders, and legal support.
⚠️ Management overhead
• Weekly or monthly cross-department meetings to review findings, action items, and risk areas.
• Time spent preparing Board reports and explaining fluctuating compliance status.
• Internal debates over how to interpret FLTCA and O. Reg. 246/22 requirements in edge cases.
It's not unusual for this to add another $30,000–$50,000 in leadership time.
When you put it all together, the “hidden” total lands somewhere between $120,000 and $310,000 per year for a single home—before you even consider the opportunity cost of tying up your best clinical minds in paperwork.
Why Traditional Approaches Are Breaking Down
Most Ontario LTC homes are using one (or a mix) of three approaches. All of them worked “well enough” before FLTCA; they're not scaling now.
The manual grind
• Leaders spend days extracting data from 30–50 page PDF inspection reports, manually listing each finding, cross-referencing FLTCA sections, and creating checklists in Word and Excel.
• Every new report means another bespoke spreadsheet, more email threads, more risk that something slips through the cracks.
• Processing time: 20–40 hours per report, with an uncomfortably high error risk when multiple people touch the same file.
The consultant dependency
• External consultants bring expertise, but at $150–$300 per hour, the costs add up quickly.
• You gain insight, but not internal capability; the knowledge walks out the door when the engagement ends.
• Over time, compliance becomes something that happens to your home, not something that's built into your operating DNA.
Generic compliance software
• Many quality systems were built for ISO, acute care, or generic risk management—not for Ontario's long-term care legislation.
• They often store documents well but don't understand FLTCA sections, Ministry inspection language, or the escalation path from written notification to AMPs and potential license implications.
• You end up bolting on spreadsheets and manual work around the software, which defeats the purpose.
All three approaches share the same flaw: they keep you in a reactive, fragmented, labour-intensive model. You're always catching up instead of getting ahead.
What the "Intelligent Algorithm Era" Actually Looks Like
The question I kept asking myself was simple: what would an inspection-ready, FLTCA-native workflow actually look like for an Ontario LTC home?
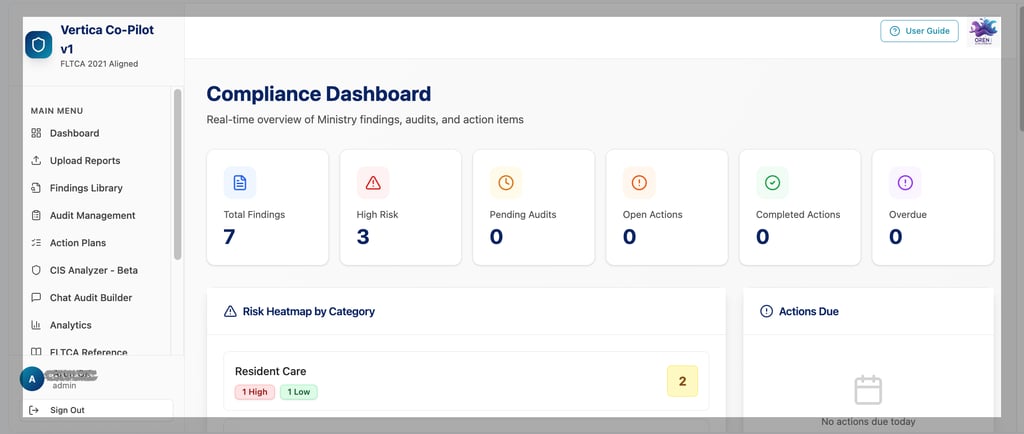
Here's the model we've built into Vertica Co‑Pilot—a purpose-built platform for FLTCA compliance that's now in active use with Ontario LTC operators.
Step 1 (Human) - Upload (2 minutes)
Frontline or leadership staff upload the Ministry inspection report as a PDF or paste the text. No formatting, no pre-work.
Step 2 (Intelligent App) - Intelligent extraction (≤30 seconds)
The system automatically detects each finding, classifies it by inspection area (for example, IPAC, medication, falls, staffing), assigns a risk level, and links it to the relevant FLTCA and O. Reg. 246/22 sections. Typical accuracy is in the mid-90% range, with human review for edge cases.
Step 3 (App with Human supervision) - Audit question generation (≤1 minute)
For each finding, Vertica Co‑Pilot generates focused audit questions structured around root causes (People, Process, Policy, Product, Environment). Each audit item includes evidence type (observation, documentation, interview, policy review), an expected standard with FLTCA-aligned language, and clear ownership (Administrator, Manager, Clinical Leader, Supervisor).
Step 4 (Human enabled by app) - Evidence collection in the field
Teams perform audits using mobile-friendly forms, upload photos and documents, and record observations at the point of care. Everything is automatically linked back to the original finding.
Step 5 (Human) - Action item automation
Non-compliant responses trigger action items with priority levels, due dates and owners, status tracking and verification, and a complete corrective-action trail that's inspection-ready.
Real-time analytics and Board-ready views
Dashboards surface compliance rates by domain and home, risk heatmaps, overdue actions, repeat finding patterns, and trend lines. Pulling a Board-ready compliance report becomes a click, not a multi-week project.
The net result: a process that took 20–40 hours per report can now be compressed into 2–5 minutes of system time plus focused human review.
The ROI: More Than Just Time Savings
When you translate this into numbers across a year, the impact becomes impossible to ignore.
⏳ Time savings
• ~90% reduction in report processing effort.
• ~85% reduction in manual audit preparation.
• ~80% reduction in time spent tracking and chasing action items.
Across a typical home, that's roughly 972 hours of work freed up annually.
💰Cost avoidance
• $40,000–$60,000 in direct labour that can be redeployed to resident-facing quality improvement.
• Reduced exposure to escalating penalties and orders by catching trends earlier and documenting corrective action more rigorously.
• $30,000–$50,000 in recovered leadership capacity for strategy, culture, and clinical excellence.
In most implementations, the payback period for a modern compliance platform is measured in months, not years—not just because of the hard ROI, but because inspections don't stop while you evaluate technology.
⚖️ the numbers, the real shift is cultural:
• Compliance becomes proactive instead of reactive.
• Workflows are standardized across homes, making multi-site leadership vastly more manageable.
• Staff understand expectations with more clarity and less fear.
• Boards gain real-time visibility instead of retrospective snapshots.
Why Vertica Co‑Pilot Is Different
There are plenty of “AI-enabled” platforms on the market right now. The ones that stick in LTC share a few common traits; Vertica Co‑Pilot was designed around those traits from day one.
✅ Purpose-built for FLTCA 2021
The platform isn't a generic healthcare quality tool adapted for long-term care. It's built specifically around Ontario's legislative and regulatory framework, including FLTCA language, Ontario inspection structures, and enforcement pathways.
✅ Algorithm-native, not an AI add-on
Intelligent extraction, audit generation, and risk detection are at the core of the system, not bolt-on features or one-off experiments.
✅ End-to-end workflow in one place
From PDF upload to Board reporting, everything happens in a single platform. No external trackers, no "export to Excel," no separate action logs.
✅ Proactive "Chat Audit Builder"
Teams can ask in plain language, "Create a monthly infection prevention audit for our memory care unit," and the system returns a full audit protocol aligned with FLTCA expectations and local best practices.
✅ Early warning and escalation insight
The platform monitors your inspection and incident history, flags patterns, and highlights when new issues fall into categories that previously led to orders or AMPs, giving you a practical early warning system before enforcement escalates.
Who Needs to Be Paying Attention
Different leaders feel this problem in different ways.
• CEOs and Board members: Need clearer oversight of compliance risk and confidence that the organization can scale without multiplying manual compliance effort.
• CFOs: Care about predictable operating costs, reduced penalty exposure, and better positioning with insurers and lenders.
• COOs and operations leaders: Need standardized workflows across homes and clear accountability that doesn't depend on one "compliance hero" per site.
• Chief Nursing/Clinical leaders: Want FLTCA alignment that supports quality improvement, not just box-checking, and need to protect their teams from burnout caused by endless documentation and rework.
The homes that will thrive under FLTCA are not necessarily the ones with the biggest budgets. They're the ones that treat compliance as a strategic capability and invest in infrastructure that turns regulatory pressure into an engine for quality.
If You're Ready to Get Out of the Manual Trap
If you're an LTC administrator, COO, or executive who feels like your team is permanently stuck in "inspection response mode," there is a different way to run this.
Typical steps we recommend:
1. Start with a single inspection report.
2. Run it through an intelligent platform like Vertica Co‑Pilot and compare the output to your last manual process.
3. Use the pilot to build your internal case: quantify time saved, risk visibility, and Board reporting improvements.
4. Roll out in 2–4 weeks; with focused training and change management, most homes can move from spreadsheets to a structured, algorithm-supported workflow in under a month.
If you want to see how this could work in your organization:
Email: info@orenaisolutions.com
Website: https://orenaisolutions.com/
What compliance challenges are keeping your team up at night in the FLTCA era? Drop a comment—I'd genuinely like to hear what you're seeing on the ground.
#LongTermCare #FLTCA2021 #ComplianceManagement #HealthcareInnovation #OntarioLTC #HealthTech #RegulatoryCompliance #HealthcareLeadership
### Sources
Ontario, Fixing Long-Term Care Act, 2021 and related offence/penalty provisions.
Sector and legal analyses describing doubled maximum fines for individuals and corporations under the FLTCA framework.